Medical evaluation
Janet Starck, MD
Physician oversight
Your treatment starts with medical review, symptom history, and a clear conversation about whether TMS is the right next step.
When medications and therapy fall short, or daily routine becomes increasingly difficult to manage, R Hope offers a compassionate, easy-to-understand TMS treatment approach. Experience real progress without the wait.
Reported outcomes
83%
report significant symptom relief
62%
experience remission
Why people reach out

Depression can affect sleep, focus, motivation, relationships, and the ability to get through everyday responsibilities. The treatment path should feel clearer, not heavier.
At R Hope, the goal is to help you understand your options, ask honest questions, and move forward only when the next step feels right.
No-pressure first conversation
Your first call is meant to answer questions and reduce uncertainty, not push you into a decision.
Clear next steps
We explain intake, insurance, evaluation, and timing in plain language so the process feels understandable.
Care built around daily life
Treatment is designed to fit around work, family, and normal responsibilities as much as possible.
Download the depression e-book for a calmer overview you can read at your own pace before deciding whether to reach out.
Included in the guide
A simple explanation of depression-related treatment questions, what TMS can look like in practice, and how to think about next steps without pressure.
Transcranial Magnetic Stimulation is FDA approved for depression and is often considered when medications or talk therapy alone have not brought enough relief.
The goal is not to overwhelm you with more complexity. The goal is to offer a treatment path that is measured, personalized, and manageable.
Beyond Medication
For many patients, TMS is the next step when medication side effects or limited results have made progress harder.
Insurance-Friendly
The clinic helps verify coverage and explain what approval can look like before you commit.
EEG-Guided Care
Assessment, EEG, and regular check-ins help keep the treatment process more tailored and more accountable.
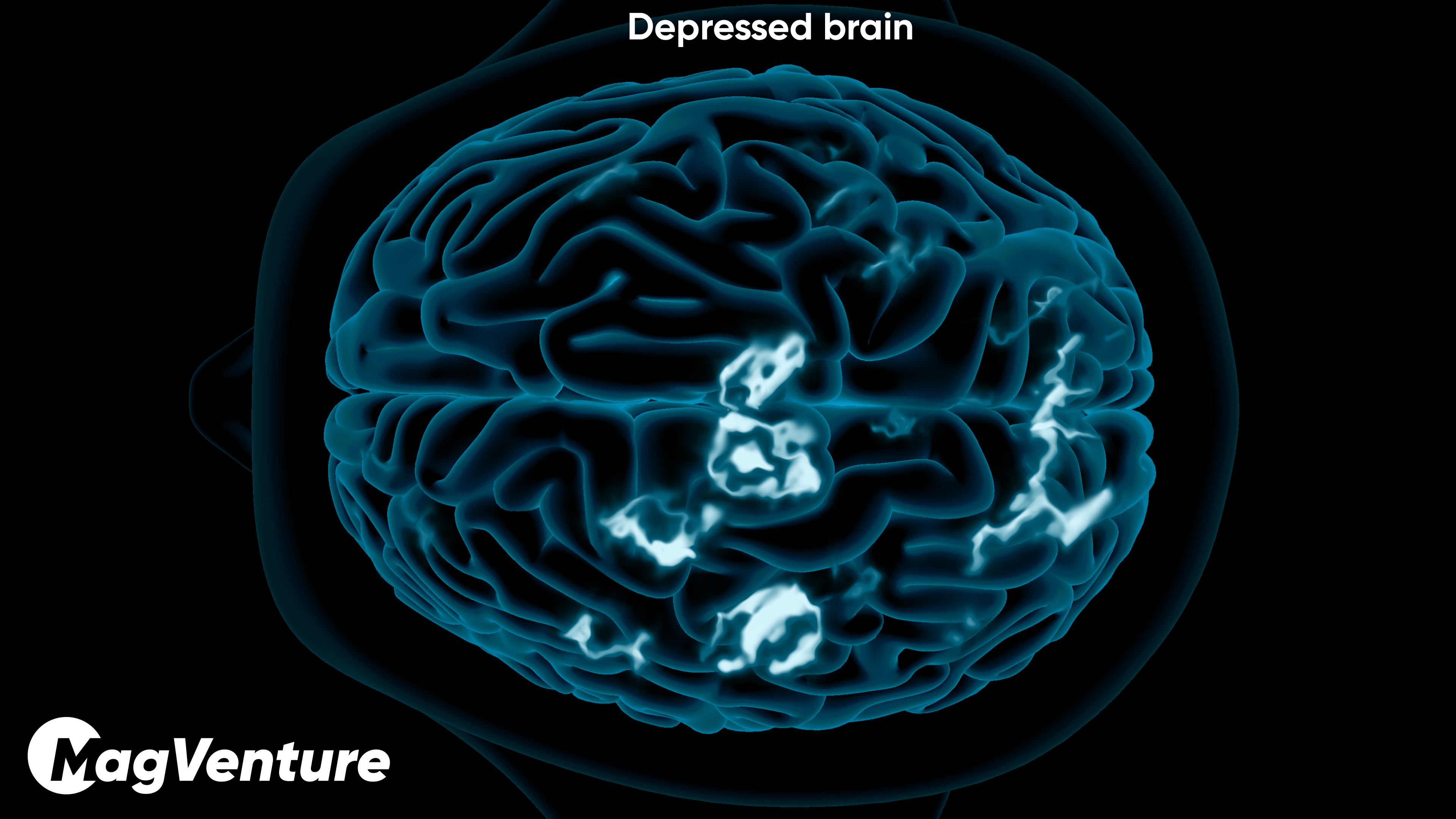
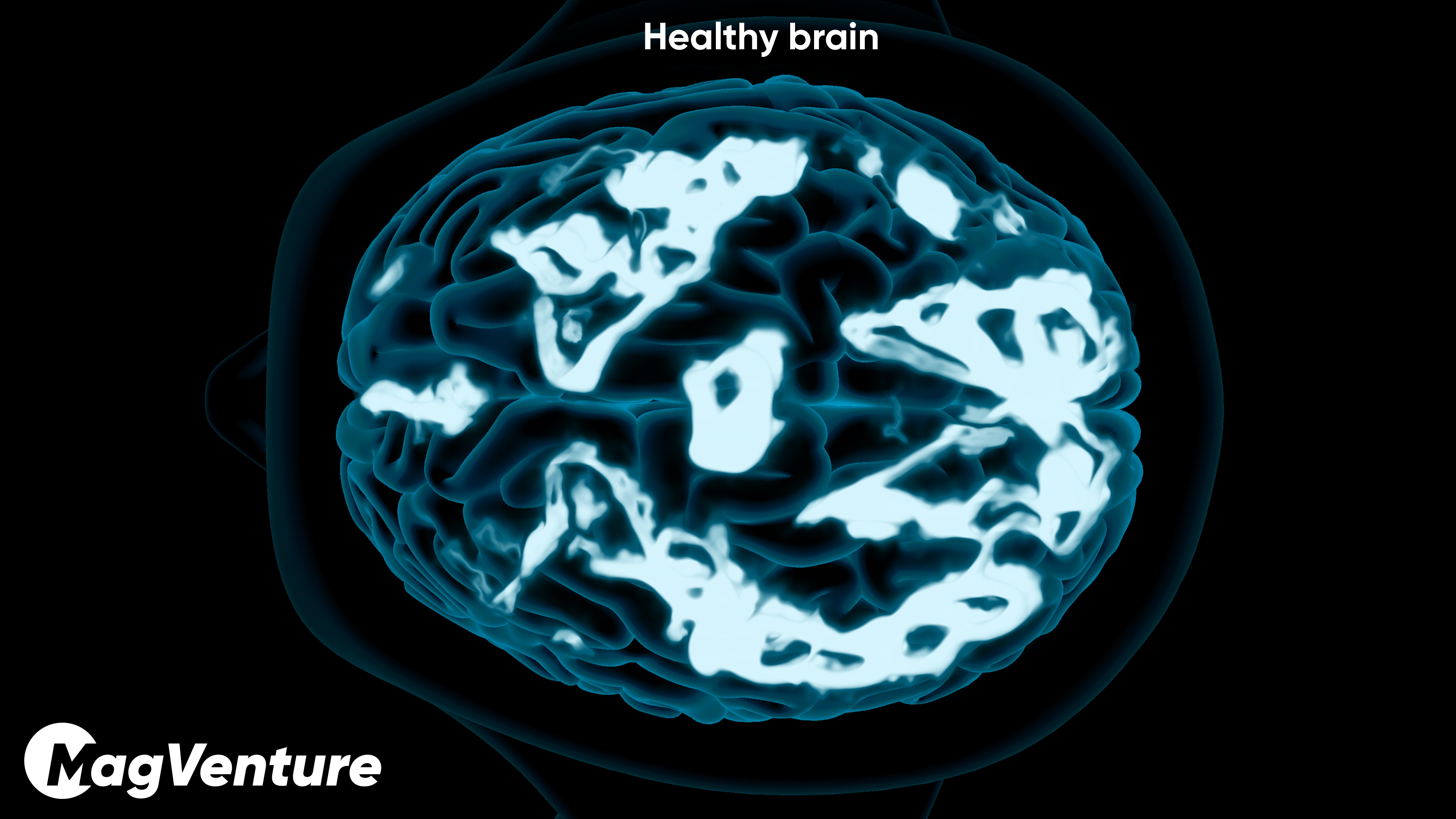
Patients are not just booking sessions. They are stepping into a treatment relationship with medical review, psychiatric oversight, and consistent day-to-day support.
Medical evaluation
Physician oversight
Your treatment starts with medical review, symptom history, and a clear conversation about whether TMS is the right next step.
Psychiatric leadership
Chief Psychiatrist and Co-Partner
Psychiatric guidance helps keep care grounded in diagnosis, safety, and long-term treatment planning.
Treatment consistency
TMS technician
From onboarding through ongoing sessions, your day-to-day treatment experience stays consistent, supportive, and easy to follow.
This is often the point where people want both better information and a place that feels safe enough to ask for help.
Many people reach out when they still feel stuck after medication, therapy, or both.
When sleep, focus, motivation, work, or relationships keep shrinking under depression, it may be time to look at another path.
People often need more than hope. They need a treatment path that feels explained, practical, and emotionally manageable.
You do not need to figure everything out alone before reaching out. We can help you understand fit, insurance, and what the first stage of treatment would involve.
From intake to ongoing progress review, the process is designed to stay clear, paced, and easy to understand.
Phase
Complete patient intake and let the clinic help review practical eligibility and insurance steps.
Phase
Your care team reviews medical history, symptoms, EEG findings, surveys, and motor threshold before sessions begin.
Phase
TMS therapy at R Hope Treatment is a step-by-step approach designed to stay practical, personalized, and easy to follow.
Phase
EEG is repeated weekly to help track improvement and synchronization of brainwaves while treatment progresses.
Every patient moves at a different pace, but this gives a clearer picture of how the first eight weeks often feel in real life.
Week 1
Get familiar with the R Hope team, technology, and your first rTMS sessions. EEG review follows every 5 sessions.
Week 2
Sessions start feeling routine while surveys and EEG help us assess early progress.
Week 3
Patients often begin feeling more relaxed and more familiar with the therapy process.
Week 4
Anxiety often starts dropping and sleep can begin to improve.
Week 5
Motivation rises and depression symptoms often begin to soften.
Week 6
Friends and family often begin noticing changes in behavior and socialization.
Week 7
Work, routines, and overall happiness often start feeling easier to manage.
Week 8
Patients are often more eager to spend time outside, feel more creative, and have more energy.
These stories are shared from the broader TMS network and reflect the kinds of changes patients often describe as treatment progresses.
"This treatment gave me a new lease on life. I am grateful for what I have in front of me now."
Nicole B., Brain Health Hawaii
Patient
"It feels like my brain is 20 years younger. Brain alertness and stamina have increased greatly. I would highly recommend it."
Mike J., Brain Health Nebraska
Patient
"I sleep through the whole night, and I feel completely rested. This treatment created a whole new outlook for me."
Daniel S., Mindset San Diego
Patient
Patient Story 01
Watch on YouTubePatient Story 02
Watch on YouTubePatient Story 03
Watch on YouTubeClinical perspective

Harold M. Koenig, MD has described TMS as one of the most significant advances he has seen in medicine.
Harold M. Koenig, MD
Vice-Admiral & Former U.S. Navy Surgeon General
Call Us
+1 (847) 868-9369Speak directly with the clinic about scheduling, insurance, and whether TMS is a fit.
Email Us
office@rhopetreatment.comSend your questions and the R Hope team will help you understand next steps.
They are minimal, but light headaches are the most common. Patients can continue daily routines without interruptions.
The most common sensation during TMS therapy is a tapping or knocking feeling on the scalp under the treatment coil. Some patients may also feel mild discomfort or a tingling sensation in the scalp area.
It depends on the insurance company, but most require a depression diagnosis, two medication trials, and failed psychotherapy. R Hope can help in this process.
This is our unique method of tracking improvement and synchronization of brainwaves. It takes only 4-5 minutes to have tangible results and follow the progress of TMS therapy.
Yes, Transcranial Magnetic Stimulation (TMS) is FDA approved for the treatment of depression in individuals who have not responded adequately to antidepressant medications.
Non-invasive, drug-free treatment tailored to your brain.
Improvements are often seen within a few weeks.